An analysis of over 800,000 women found no association between menopausal hormone therapy and increased mortality [1].
A controversial therapy
One of the first major changes that women undergo as they age is menopause, which usually occurs between 45 and 55 years of age. Menopause not only marks the end of reproduction, the hormonal changes that accompany it are associated with declines in cognition, cardiovascular health, and other unpleasant symptoms that affect around 80% of women, such as hot flushes, night sweats, and decreased libido [2, 3]. Menopause also has a profound impact on the economy, with menopause-related unemployment having an estimated $2.1bn (£1.5bn; €1.7bn) impact annually in the United Kingdom alone [4].
Menopausal hormone therapy containing the sex hormone estrogen can reduce menopause-related symptoms; however, its use has recently decreased due to safety concerns [5, 6]. Those concerns were raised by the 2002 Women’s Health Initiative study, which linked hormone replacement therapy to a higher risk of breast cancer, heart attack, stroke, and blood clots [7]. However, this study had a major caveat: the participants were, on average, 63 years old at enrolment, well past menopause.
Other studies, investigating women who are just before menopause (perimenopausal) and are younger compared to the Women’s Health Initiative study, paint a different picture. For example, in a review that we have recently covered, the authors examined a broad range of studies assessing the risks and benefits of hormone replacement therapy. They suggested that, while the risk-benefit ratio should be evaluated on an individual basis, hormone replacement therapy could be used as a geroprotector to extend women’s healthspan.
Similarly, previous studies also suggest that menopausal hormone therapy use leads to either a reduction or no change in mortality [8-10]. However, as the authors of this study suggest, those studies have many shortcomings, such as data having unknown treatment durations or samples that are too small.
A robust dataset
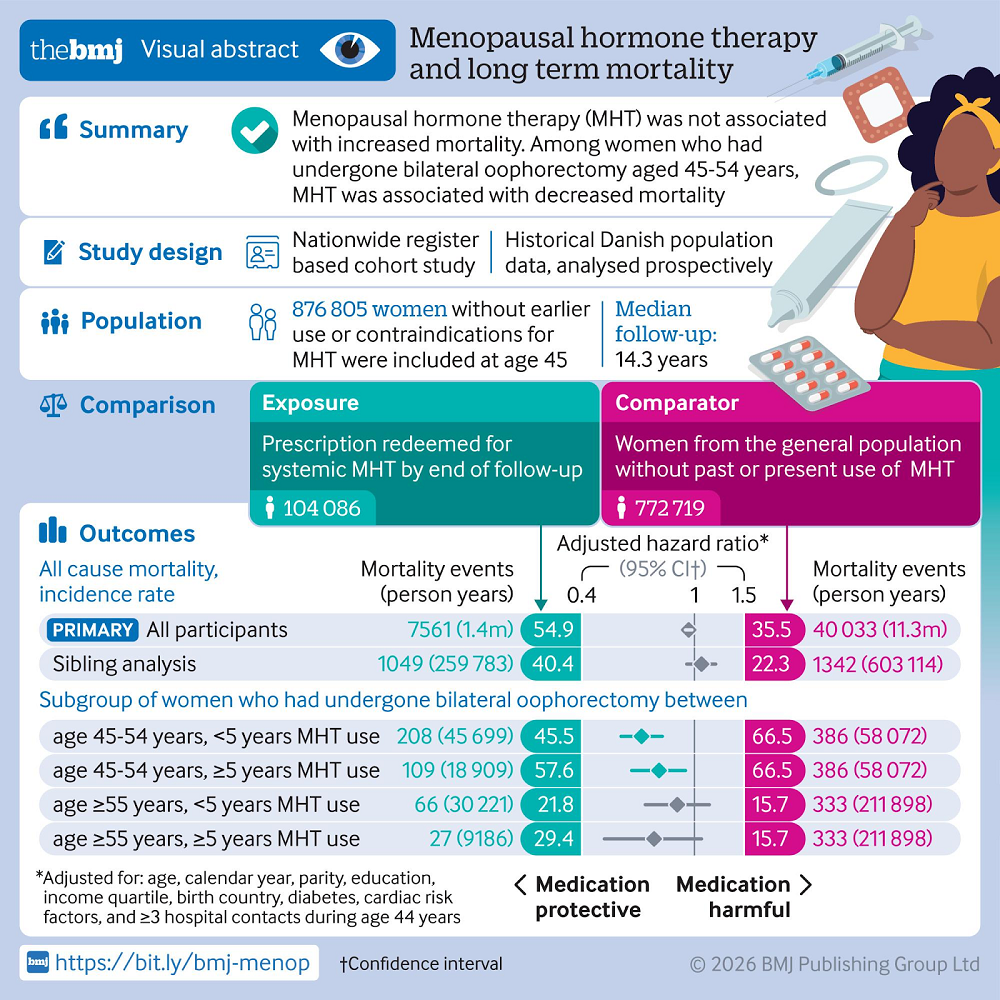
To address this, the authors of this study used nationwide Danish registers to obtain data from over 800,000 women born between 1950 and 1977 and living in Denmark on their 45th birthdays. This study excluded women with any risk factors for menopausal hormone therapy (except for the primary analysis; however, this exclusion didn’t change the conclusions), women who started using menopausal hormone therapy before age 45, and women who underwent surgical removal of the ovaries (oophorectomy). Participants were followed up for 7 to 21 years. The authors used this data to determine whether menopausal hormone therapy increases the risk of all-cause mortality.
Among the participants, almost 12% were exposed to menopausal hormone therapy. The type of hormone used varied among participants; however, the most common were tablets containing estradiol and continuous norethisteronacetat. Median treatment duration, recorded at the end of the follow-up period, was short (1.7 years), and fewer than 1% of women reported 10 or more years of use.
There were some differences between groups of women who took and didn’t take hormone replacement therapy. Those who did take the therapy, on average, “had delivered slightly fewer children, were more often divorced, had hypertension, had three or more hospital contacts between age 44 and 45, and had previously undergone hysterectomy and/or bilateral oophorectomy” (removal of uterus or ovaries) compared to women who did not.
Neutral or beneficial?
The researchers did not find an association between menopausal hormone therapy use and increased mortality. When looking at specific causes of death, no significant difference was found for long-term (≥5 years) menopausal hormone therapy use for either cardiovascular or cancer mortality, and only a modest change for short-term (<5 years) use of menopausal hormone therapy.
The lack of association between menopausal hormone therapy and increased risk of mortality was also observed when the researchers compared data from siblings, where at least one sister used the therapy and one didn’t. This analysis minimized the impact of unmeasured confounding factors, as siblings are more likely to have similar lifestyles than the general population.
When analyzing a subgroup of women who underwent bilateral oophorectomy between 45 and 54 years, they observed 27-34% lower mortality risk, dependent on the duration of use, among women who used menopausal hormone therapy compared to those who didn’t. For women who underwent a hysterectomy, no significant increase in mortality was found.
Those findings are similar to other previous studies and agree with the guidelines from the Royal College of Obstetricians and Gynaecologists, which recommend “offering hormone therapy to all women who undergo bilateral oophorectomy before menopause, until the average age of natural menopause is reached (about 51 years), provided there are no contraindications” [11].
Hormone replacement therapy is not a uniform therapy, and its dosage and administration can vary. The authors, therefore, divided women who underwent therapy into categories and noted that lower mortality, as compared with never having used menopausal hormone therapy, was observed in groups who used transdermal menopausal hormone therapy formulations, such as plaster or gel; used estrogen monotherapy or estrogen with cyclic progesterone; or started menopausal hormone therapy at age 52 or older.
They also noted that the side effects of hormone replacement therapy do not necessarily occur after the use but during the therapy. To investigate this, the researchers completed a separate analysis by excluding women at menopausal hormone therapy cessation and found that, in this case, menopausal hormone therapy was associated with a significantly reduced mortality. While this might suggest hormone replacement benefits that cease after the therapy is discontinued, there is also a possibility of healthy user bias. Therefore, these results should be interpreted with caution.
Strengthening support for the current policy
The findings of this study add evidence in support of the Endocrine Society’s guidelines, which “recommend menopausal hormone therapy for women who have recently begun menopause who have moderate to severe symptoms and no contraindications” [12].
Literature
[1] Mikkelsen, A. P., Bergholt, T., Lidegaard, Ø., & Scheller, N. M. (2026). Menopausal hormone therapy and long term mortality: nationwide, register based cohort study. BMJ (Clinical research ed.), 392, e085998.
[2] El Khoudary, S. R., Greendale, G., Crawford, S. L., Avis, N. E., Brooks, M. M., Thurston, R. C., Karvonen-Gutierrez, C., Waetjen, L. E., & Matthews, K. (2019). The menopause transition and women’s health at midlife: a progress report from the Study of Women’s Health Across the Nation (SWAN). Menopause (New York, N.Y.), 26(10), 1213–1227.
[3] Avis, N. E., Crawford, S. L., Greendale, G., Bromberger, J. T., Everson-Rose, S. A., Gold, E. B., Hess, R., Joffe, H., Kravitz, H. M., Tepper, P. G., Thurston, R. C., & Study of Women’s Health Across the Nation (2015). Duration of menopausal vasomotor symptoms over the menopause transition. JAMA internal medicine, 175(4), 531–539.
[4] NHS Confederation. Women’s health economics: investing in the 51 per cent.
[5] Yang, L., & Toriola, A. T. (2024). Menopausal Hormone Therapy Use Among Postmenopausal Women. JAMA health forum, 5(9), e243128.
[6] Ameye, L., Antoine, C., Paesmans, M., de Azambuja, E., & Rozenberg, S. (2014). Menopausal hormone therapy use in 17 European countries during the last decade. Maturitas, 79(3), 287–291.
[7] Rossouw, J. E., Anderson, G. L., Prentice, R. L., LaCroix, A. Z., Kooperberg, C., Stefanick, M. L., Jackson, R. D., Beresford, S. A., Howard, B. V., Johnson, K. C., Kotchen, J. M., Ockene, J., & Writing Group for the Women’s Health Initiative Investigators (2002). Risks and benefits of estrogen plus progestin in healthy postmenopausal women: principal results From the Women’s Health Initiative randomized controlled trial. JAMA, 288(3), 321–333.
[8] Grodstein, F., Stampfer, M. J., Colditz, G. A., Willett, W. C., Manson, J. E., Joffe, M., Rosner, B., Fuchs, C., Hankinson, S. E., Hunter, D. J., Hennekens, C. H., & Speizer, F. E. (1997). Postmenopausal hormone therapy and mortality. The New England journal of medicine, 336(25), 1769–1775.
[9] Holm, M., Olsen, A., Au Yeung, S. L., Overvad, K., Lidegaard, Ø., Kroman, N., & Tjønneland, A. (2019). Pattern of mortality after menopausal hormone therapy: long-term follow up in a population-based cohort. BJOG : an international journal of obstetrics and gynaecology, 126(1), 55–63.
[10] Manson, J. E., Aragaki, A. K., Rossouw, J. E., Anderson, G. L., Prentice, R. L., LaCroix, A. Z., Chlebowski, R. T., Howard, B. V., Thomson, C. A., Margolis, K. L., Lewis, C. E., Stefanick, M. L., Jackson, R. D., Johnson, K. C., Martin, L. W., Shumaker, S. A., Espeland, M. A., Wactawski-Wende, J., & WHI Investigators (2017). Menopausal Hormone Therapy and Long-term All-Cause and Cause-Specific Mortality: The Women’s Health Initiative Randomized Trials. JAMA, 318(10), 927–938.
[11] Manchanda, R., Gaba, F., Talaulikar, V., Pundir, J., Gessler, S., Davies, M., Menon, U., & Royal College of Obstetricians and Gynaecologists (2022). Risk-Reducing Salpingo-Oophorectomy and the Use of Hormone Replacement Therapy Below the Age of Natural Menopause: Scientific Impact Paper No. 66 October 2021: Scientific Impact Paper No. 66. BJOG : an international journal of obstetrics and gynaecology, 129(1), e16–e34.
[12] Stuenkel, C. A., Davis, S. R., Gompel, A., Lumsden, M. A., Murad, M. H., Pinkerton, J. V., & Santen, R. J. (2015). Treatment of Symptoms of the Menopause: An Endocrine Society Clinical Practice Guideline. The Journal of clinical endocrinology and metabolism, 100(11), 3975–4011.
View the article at lifespan.io








































