https://www.ncbi.nlm...8258794/related
This is not mice study. It is human data.
Edited by MikeDC, 26 September 2017 - 11:40 PM.

Posted 26 September 2017 - 11:39 PM
Edited by MikeDC, 26 September 2017 - 11:40 PM.
Posted 26 September 2017 - 11:58 PM
FULL TEXT:
Posted 27 September 2017 - 12:03 AM
This is not mice study. It is human data.
It's also an associational study: it does not prove causality.
"These findings provide evidence for redox imbalance in the brain in all phases of SZ, potentially reflecting oxidative stress." There's no finding of reduced NAD+ or total NAD(H), but of a shift in NAD+:NADH poise. Their interpretation — and it's a reasonable one — is not that schizophrenics suffer from low NAD+, but that schizophrenics suffer from high oxidative stress, which then skews the NAD+:NADH.
Posted 27 September 2017 - 02:37 PM
Study says the problem is the balance between NAD+ and reduced NADH, not low NAD+.
Will increasing NAD+ through precursors improve the situation? I have no idea.
Posted 27 September 2017 - 02:44 PM
Posted 27 September 2017 - 02:51 PM
I suppose it depends on the rate that NAD+ is getting reduced. If that rate is not limited then simply increasing NAD+ may not affect the ratio that much.
The real proof of the pudding is in the eating. Someone needs to dose some schizophrenia patients with NR and see if they improve. Then you'd have a real answer instead of speculation.
Posted 27 September 2017 - 03:00 PM
Posted 27 September 2017 - 03:16 PM
Posted 27 October 2017 - 02:30 PM
The study I link to below is not about NR or a human clinical trial. The authors research skin fibroblasts of young humans, those of healthy old humans and those of Late Onset Alzheimers Disease (LOAD). On the basis of their findings they argue that LOAD is not only caused by multifactorial 'clumpings' in the brain but also by low NAD+ and impaired mitochondrial metabolism. They do not mention NR or other precursors but it seems likely to me that taking such precursors will play a role in combating LOAD. I am ApOE4 hetero myself, so I am once again glad that I have been taking moderate amounts of NR for some years now...
https://www.nature.c...98-017-14420-x
Edited by Harkijn, 27 October 2017 - 02:31 PM.
Posted 27 October 2017 - 06:04 PM
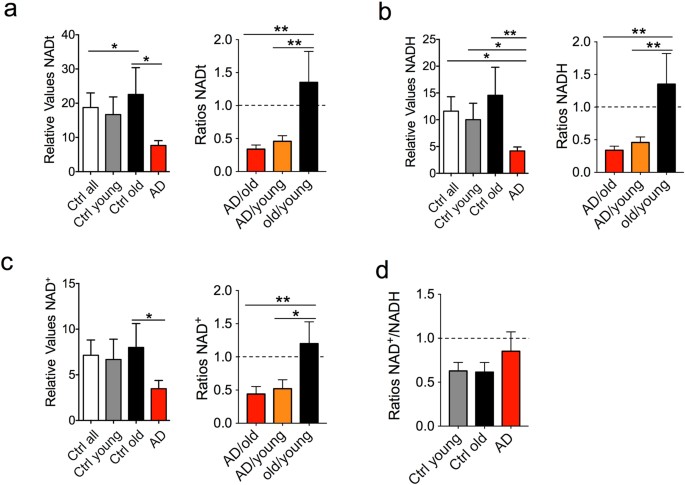
The authors research skin fibroblasts of young humans, those of healthy old humans and those of Late Onset Alzheimers Disease (LOAD). On the basis of their findings they argue that LOAD is not only caused by multifactorial 'clumpings' in the brain but also by low NAD+
They actually report some things that are the opposite of what you'd expect from the general story of the redox shift to low NAD:NADH in aging we've seen reported elsewhere: "Nicotinamide metabolites, including [total NAD+ + NADH] (a), NADH (b), and NAD+ (c) were decreased in LOAD samples compared to young and old controls, while the RRs (ratios NAD+/NADH) were not different between controls, but slightly increased in LOAD fibroblasts compared to all, young, and old control cells"
Edited by Michael, 27 October 2017 - 06:11 PM.
Posted 27 October 2017 - 08:22 PM
Posted 31 October 2017 - 09:41 PM
If the data doesn't match the theory, and the data has been well verified, then time to change the theory.
Posted 06 January 2018 - 03:28 PM
A quick search on the lead author's name leads me to think that this study has not yet been mentioned in the forums:
http://www.jbc.org/c...1/20/10836.full
It is a very upbeat account of reversing toxicity in ALS astrocytes by raising NAD+levels. The authors used NMN in their research and seem to prefer it slightly to NR, but explicitly conclude that NMN and NR (as well as overexpressing NAMPT) are beneficial in vitro.
Posted 06 January 2018 - 05:47 PM
This is not mice study. It is human data.
It's also an associational study: it does not prove causality.
"These findings provide evidence for redox imbalance in the brain in all phases of SZ, potentially reflecting oxidative stress." There's no finding of reduced NAD+ or total NAD(H), but of a shift in NAD+:NADH poise. Their interpretation — and it's a reasonable one — is not that schizophrenics suffer from low NAD+, but that schizophrenics suffer from high oxidative stress, which then skews the NAD+:NADH.
Then reducing ROS in the brain would seem to allow for homeostatic response.
I wonder if high dose liposomal vitamin C (10-20 grams per day) would result in amelioration of SZ symptoms.
It couldn't hurt unless the subjects suffer from rare mutation that causes hemolytic anemia from megadoses of ascorbate ( G6PD Deficiency)
0 members, 1 guests, 0 anonymous users