.
O P E N A C C E S S S O U R C E : Aging and Drug Discovery
Abstract
Nicotinamide adenine dinucleotide (NAD) pharmacology is a promising class of treatments for age-related conditions that are likely to have a favorable side effect profile for human use, given the widespread use of the NAD precursor vitamin B3 supplements. However, despite several decades of active investigation and numerous possible biochemical mechanisms of action suggested, only a small number of randomized and adequately powered clinical trials of NAD upregulation as a therapeutic strategy have taken place. We conducted a systematic review of the literature, following the PRISMA guidelines, in an attempt to determine whether or not the human clinical trials performed to date support the potential benefits of NAD supplementation in a range of skin, metabolic and age-related conditions. In addition, we sought medical indications that have yielded the most promising results in the limited studies to date. We conclude that promising, yet still speculative, results have been reported for the treatment of psoriasis and enhancement of skeletal muscle activity. However, further trials are required to determine the optimal method of raising NAD levels, identifying the target conditions, and comparisons to the present standard of care for these conditions. Lastly, pharmacological methods that increase NAD levels should also be directly compared to physiological means of raising NAD levels, such as exercise programs and dietary interventions that are tailored to older individuals, and which may be more effective.
1. Introduction
The cofactor nicotinamide adenine dinucleotide (NAD) is an important metabolic regulator of cellular redox reactions and a co-factor or a co-substrate for key enzymes essential for normal cellular function in different tissues. Known as NAD+ in its oxidized state and NADH in its reduced state, it was first described more than a century ago as a molecule in the electron transport chain in the metabolic reduction-oxidation reactions in mitochondria [1]. Poly(ADP-ribose) polymerases (PARPs), a group of enzymes that catalyze the transfer of ADP-ribose to target proteins, use NAD as a cofactor [2]. PARPs regulate many important cellular functions, including expression of transcription factors, gene expression and DNA repair. More recent interest in NAD emerged from research into the role of sirtuins, NAD-dependent deacylases, after the discovery that Sirtuin 2 is an NAD+-dependent histone deacetylase [3]. Sirtuins influence many important cellular processes, including inflammation, bioenergetics, circadian rhythm generation, and cell growth, all fundamental to cellular aging. These pathways place NAD at the center of cellular metabolism, mitochondrial function, and biological processes of aging.
Most human cells must rely on de novo creation of NAD from a variety of building blocks (Figure 1) [4]. NAD can be synthesized de novo from tryptophan via the kynurenine pathway or from nicotinic acid via the Preiss-Handler pathway [5]. However, the bulk of NAD synthesis in cells is generated via the NAD salvage pathways acting on the precursor molecule nicotinamide. Nicotinamide, the dominant NAD precursor, originates from the diet or can be produced by the activity of a variety of NAD hydrolases that include CD38/CD157, PARPs and Sirtuins [6].
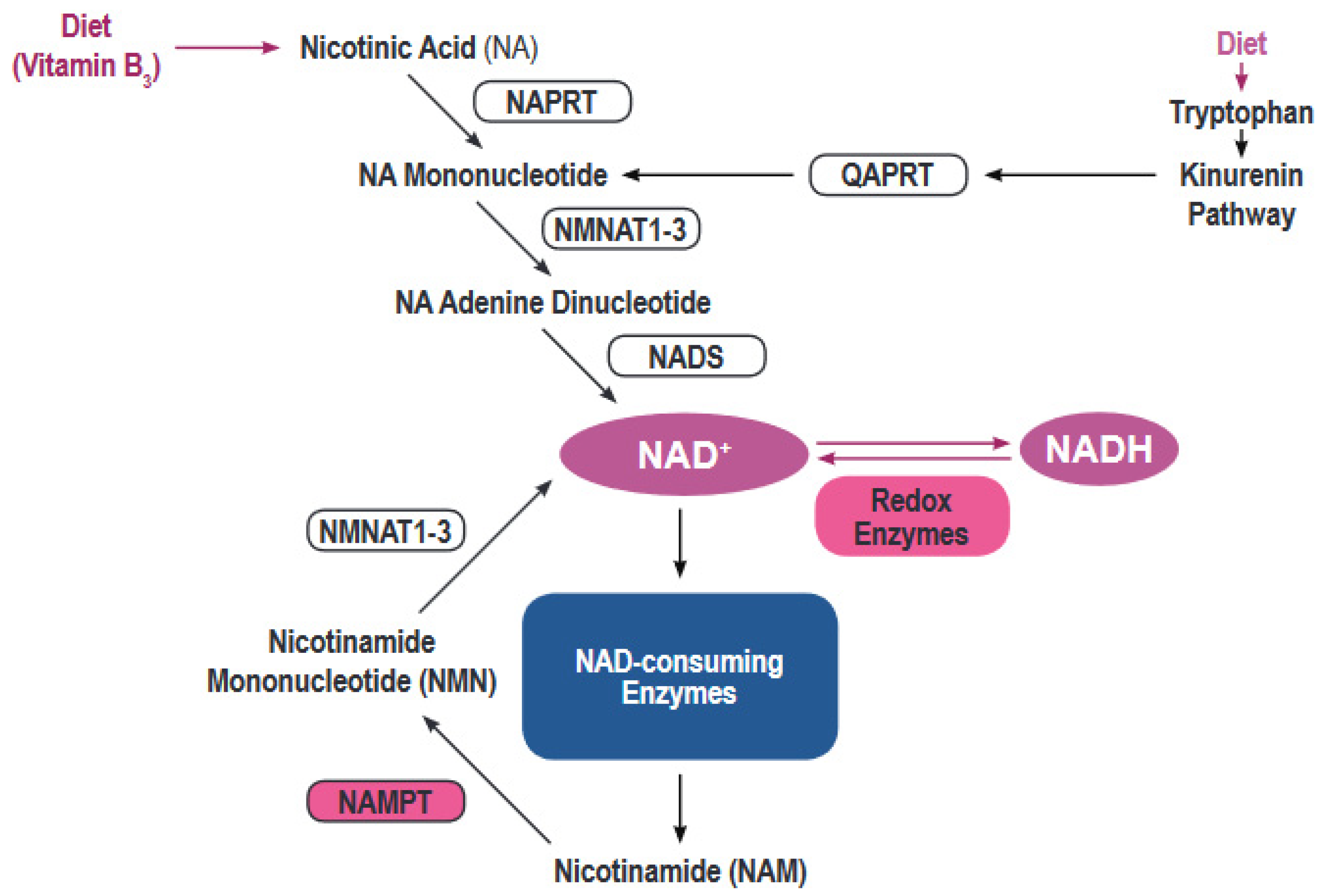
Figure 1. Regulation of the nicotinamide adenine dinucleotide (NAD) metabolism. The figure shows the main synthesis pathways of NAD including the de novo synthesis via the kynurenine pathway or from nicotinic acid and the salvage pathways.
NAD levels decline with increasing age, as the activities of both the salvage pathways and de novo synthesis are reduced, the result of altered levels of rate-limiting enzymes and precursors. There is also growing evidence that the activity of specific NAD hydrolases, particularly CD38, increases in specific tissues during aging [7]. Evidence from animal studies indicates that interventions that increase NAD levels produce numerous benefits on the overall cardiometabolic health and immune function [4]. A fall in NAD levels might be prevented with supplementation with NAD precursors, such as nicotinamide, nicotinic acid, nicotinamide mononucleotide (NMN), and nicotinamide riboside (NR). NMN and NR are believed to be orally bioavailable and feed into the NAD salvage pathway directly (NMN) or indirectly (NR via NMN) and thereby bypass a key rate-limiting step determined by the enzymatic activity of NAMPT which decreases with age. Both NMN and NR have received the most recent interest as promising future therapeutic strategies to raise NAD levels [8].
However, supplementation with NAD precursors is not the only way to increase NAD levels. Other possible approaches include strength training [9], upregulation of critical enzymes (e.g., rate-limiting NAMPT) involved in NAD salvage [10], and inhibiting NAD degradation (e.g., with bioavailable flavonoids to inhibit CD38) [11].
Evidence suggesting the benefits of NAD upregulation in humans has accumulated, but much of it involves the use of vitamin B3 and predates the most recent sirtuin-related expansion of knowledge of the role of NAD in cellular metabolism and aging. For example, daily niacin intake has been recommended for much of the past century. Furthermore, extensive literature already accompanies the use of high-dose niacin for dyslipidemias in the context of cardiovascular disease prevention [12,13]. However, the literature currently lacks a rigorous assessment of the potential role of NAD upregulation on healthspan using relevant surrogate biomarkers of aging.
A number of clinical trials have been conducted recently, with more underway, to rigorously assess NAD pharmacology in the context of aging and metabolic and age-related disease. These trials benefit from the more recent understanding of NAD and its relationships with important processes in cellular aging, and so NAD has been discussed as a therapeutic intervention for a range of age-related conditions, including immune decline (immunosenescence) and sterile chronic inflammation (inflammaging). De novo NAD synthesis is involved in the innate immune response of macrophages [14] and, indeed, the broader immune response, due to elevated cellular energy requirements during an acute immune response [15,16].
More recently, NAD upregulation has been proposed as a prevention or treatment of viral illnesses and vaccine boosters. These are of particular interest for treating COVID-19, a new disease caused by the novel SARS-CoV-2 coronavirus. The elderly are at increased risk of mortality and morbidity of the COVID-19 infection, and pharmacological enhancement of NAD levels, which might have a beneficial effect on the biological processes of aging, might be particularly useful in this context. Thus far, no evidence of benefit has been reported, and it remains unclear as to whether upregulating NAD is an effective therapy for immune decline. Animal studies have suggested a double-edged sword situation regarding NAD and immunity where raising NAD levels might lead to increased activity of immune cells in inflammatory conditions [15,17].
Considering all of the above, we have conducted a review of the literature in an attempt to determine whether or not the present human evidence for the potential benefits from NAD pharmacology supports an expansion of efforts to assess this approach to age-related conditions.
2. Methods
.../...
3. Results
3.1. Screening
In the initial screen, 289 records were identified. All were reviewed to ensure relevance and full-text availability. Of these, 36 records met the eligibility requirements. The characteristics of these studies are summarized in Table 1, in that the authors reported human trial data for interventions based on NAD pharmacology.
Table 1. Studies of NAD pharmacology and related interventions.
Table 2. Selected clinical trials yet to publish results.
3.2. Summary of Studies
Of the 36 human trials with published results identified in our literature review, 18 reported on oral administration of NAD precursors, such as nicotinamide, NMN, or NR, while 8 employed oral administration of NAD. The remainder used an eclectic mix of exercise programs, antioxidants, forms of topical, intravenous, or intramuscular administration of NAD, as well as compounds targeting NQO1 activity. Of the 36 trials, 7 assessed only pharmacokinetics, safety, or biomarkers, and 17 reported beneficial outcomes. The remaining 12 reported no benefits to patients.
Our review reveals that the upregulation of NAD has been studied for a wide range of medical conditions, only a few of which are addressed by more than one study. These conditions include acute kidney injury, Alzheimer’s disease, chronic fatigue syndrome, dementia, hyperphosphatemia, hypertension, obesity, Parkinson’s disease, photoaging of skin, psoriasis, skin cancers, type 1 diabetes mellitus, type 2 diabetes mellitus, and schizophrenia.
NAD levels after intervention were measured in only 11 trials, in blood samples or tissues, via quantitative methods such as colorimetric analysis. In all cases, increased NAD was observed, but the size of the effect varied widely. These changes were almost incomparable due to the current lack of standardization, as variance may be due to differences in methodology of measurement, in interventions, or other factors.
Of the completed, published trials identified in this study, only two were adequately powered. Firstly, the European Nicotinamide Diabetes Intervention Trial that employed daily supplementation of nicotinamide. The primary outcome of progression to type 1 diabetes was negative [29]. Secondly, the open-label trial of oral and infused NADH in Parkinson’s disease patients by Birkmayer et al. showed a beneficial effect in 80% of the patients [23]. The effects on NAD in serum or tissues were assessed in neither of these studies. It should also be noted that the metabolism of intravenously infused NAD/NADH is currently unclear although it is likely that both metabolites are cleaved into nicotinamide and ADP-ribose by the liver, as has been demonstrated in mice [53]. It is also possible that CD38-expressing cells, such as leukocytes [54], act to degrade NAD/NADH in plasma.
3.2.1. Neurological and Neurodegeneration Conditions
The earliest deliberate attempts at NAD pharmacology, as distinct from the extensive study of vitamin B3, involved the delivery of niacin or formulations of NAD in the treatment of schizophrenia, beginning in the 1960s [18,19,20]. This intervention was based on a variety of hypotheses linking NAD biochemistry to the neurobiological changes thought to be involved in schizophrenia. More modern hypotheses of NAD-related redox dysfunction in schizophrenia continue to be debated today; mitochondrial dysfunction and oxidative stress are thought to contribute to the pathogenesis of the condition [55]. Available reports refer to positive results in earlier studies, but the authors reported no benefits to patients resulting from their small clinical trials.
Beginning in the 1990s, NAD pharmacology was assessed as a basis for the treatment of Parkinson’s disease and Alzheimer’s disease [22,23,24,25], efforts that have since expanded to other forms of dementia [56]. To date, the results of clinical trials have been mixed for Parkinson’s disease and largely negative for Alzheimer’s disease. Further trials are in progress.
3.2.2. Skin Conditions
NAD upregulation prevents actinic keratosis and improves some measures of photoaging [33,40]. While the mechanisms of action are not fully understood, NAD is a co-factor for the PARP enzymes that play a key role in DNA repair. Skin is exposed to UV damage, causing frequent DNA breaks. Improving PARP function, and thus improving DNA repair, might protect from precancerous skin lesions and other consequences of photoaging. This mechanism may also influence the skin pathology associated with dysregulated skin cell division in conditions, such as psoriasis [32].
3.2.3. Metabolic Conditions
Only limited data are available for the use of NAD boosters in the treatment of metabolic conditions, such as obesity and metabolic syndrome. While some studies report improvement in lipid profile, exercise capacity, and muscle fiber composition despite a sedentary lifestyle [37,49], others show no benefit of supplementation in the prevention of type 1 diabetes [29], and no improvements in insulin resistance [44,47].
3.2.4. Potential Side Effects
No study reported severe side effects, supporting the thesis that these interventions are likely to be relatively safe for human use. Multiple widely used over-the-counter supplements increase NAD levels, including niacin, NR, and NMN, and vitamin B3 supplementation have been in use for many years. Thus, it seems likely that side effects linked to interventions that target NAD metabolism more likely arise from impurities rather than the supplements themselves, since this industry generally operates without rigorous control of quality and standardization.
In short term experiments, high doses of nicotinamide cause hepatic toxicity [57]. High doses of niacin cause headaches, skin flushing, and dizziness [58]. These effects occur at doses much higher than those used in clinical trials and have so far not been reported in the limited number of studies of NAD pharmacology to date.
Long-term side-effects of NAD upregulation, harder to detect and quantify, may exist and sustained high doses of vitamin B3 compounds may have long-term side-effects. Excessive intake of niacin or nicotinamide may contribute to the development of Parkinson’s disease [57]. Nicotinamide may contribute to the development of diabetes, but animal data here contradict the human trial results showing no such effect [57]. Additionally, high doses of NR aggravate insulin resistance and produce white adipose tissue dysfunction in mice [59].
Another possible concern following chronic high-level administration of nicotinamide is the depletion of methyl groups. It has been reported that nicotinamide induces nicotinamide-N-methyltransferase which catalyzes the methylation of nicotinamide. This may cause secondary problems by consuming methyl groups that are required elsewhere to maintain cellular homeostasis [60].
NAD upregulation may also worsen the senescence-associated secretory phenotype (SASP) produced by senescent cells in old tissues. A proposed mechanism for this side-effect involves suppression of AMPK and p53, leading to stimulation of NF-κB via p38 MAPK and increased expression of inflammatory cytokines [61]. The burden of cellular senescence increases with age, and the SASP contributes to diverse pathologies of aging [62] An alternative hypothesis is that activation of a stronger SASP by NAD boosters may lead to enhanced clearance of senescent cells and an anti-aging effect, but supporting data, in either case, is presently very limited.
Supporting evidence for these potential long-term issues is sparse at best and entirely lacking in some cases. Given the fact that anti-aging interventions are likely to target comparatively healthy, comparatively younger individuals, quantification of potential long-term adverse effects will be critical to ensure that these interventions are safe.
4. Discussion
NAD is required for critical cellular pathways involving NAD-consuming enzymes (sirtuins, PARPs and CD38) and NAD-utilizing but non consuming enzymes (using the NAD/NADH redox couple). These two classes of enzymes rely on effective NAD levels, giving this latter metabolite a broad influence over cellular biochemistry relevant to health, disease and aging.
4.1. Gaps in the Knowledge of NAD
NAD levels decrease with age in tissues throughout the body. While numerous mechanisms have been proposed to explain this observation, there is still only an incomplete understanding of this phenomenon. Investigations of NAD biochemistry have largely focused on proximate causes, meaning changes in the expression of proteins that are rate-limiting in NAD synthesis and salvage pathways. For example, nicotinamide phosphoribosyltransferase (NAMPT) levels fall with age, and NAMPT is the rate-limiting enzyme for the pathway responsible for synthesizing NAD from nicotinamide [63].
.../...
.































 This topic is locked
This topic is locked















